
Photo by Beacon Communications
The following article was written by Sarah Channing, Thrive's Director of Development & Digital Media and published on January 13, 2021 by the Cranston Herald.
Nursing our community through COVID
Throughout the pandemic, there has been no reprieve in demand for behavioral health services – and no respite for frontline workers providing direct care to clients. This is particularly true among Thrive’s nursing staff, whose responsibilities include managing the interface between primary and behavioral health care. What follows is a look at their perspectives.
“We halted everything as soon as we figured out that we were in a real pandemic, especially with our clients, stopping them from going to their day programs,” shared Mary Kenney, RN, who assists adults living in a supported housing environment. “It was a total restructure of what we had been doing.”
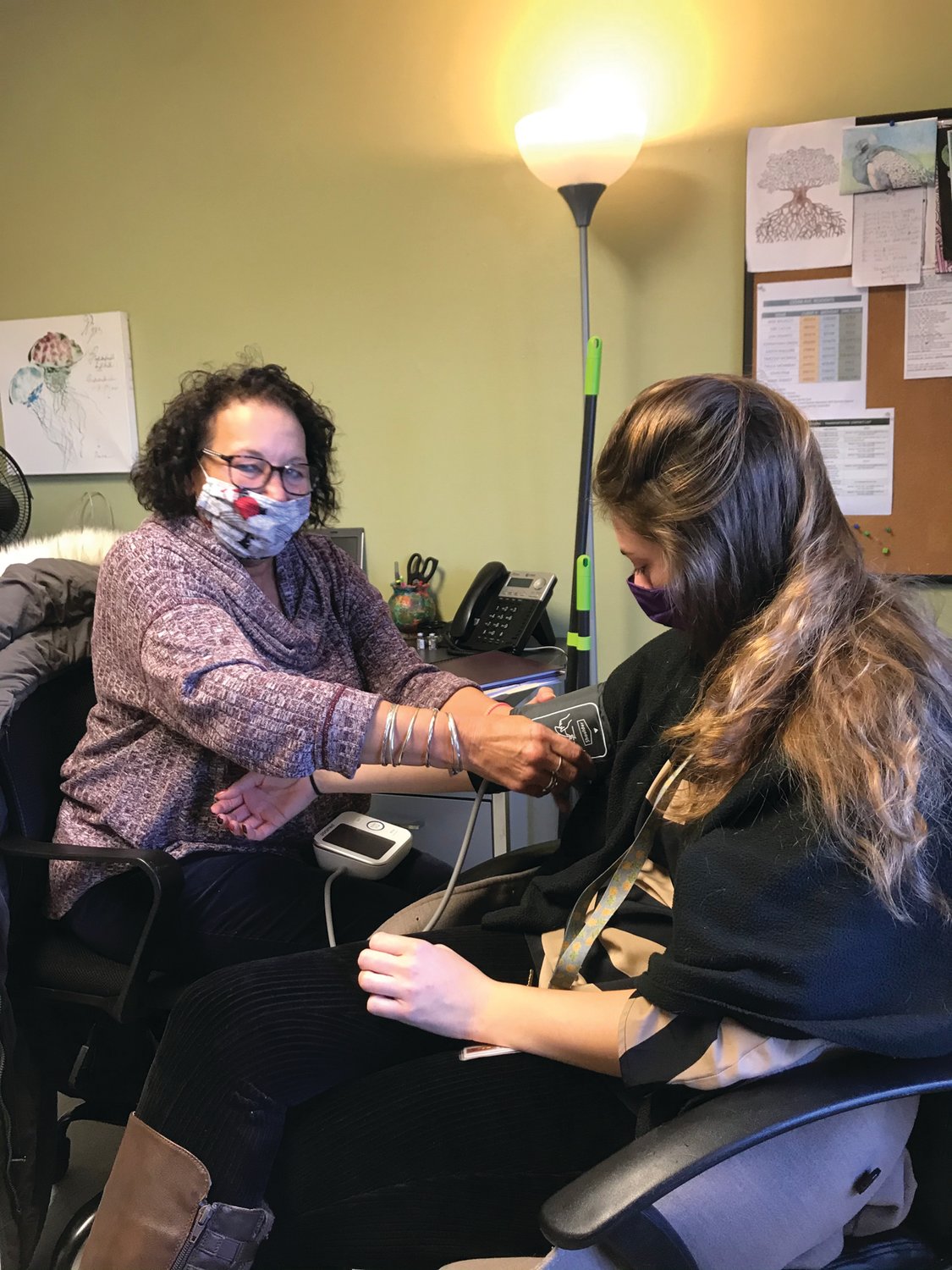
RN Mary Kenney takes Group Home Team Leader
Carly McGee’s blood pressure.
Kenney addresses her clients’ anxieties by validating their feelings. “Everybody was so fearful about what would happen to us, including myself,” she said. “I told them, it’s OK to be afraid. You’re going to feel like you don’t know what to do, but we will figure it out as we go along. If we are super careful and follow the guidelines of washing, sanitizing, wearing masks, we will survive.”
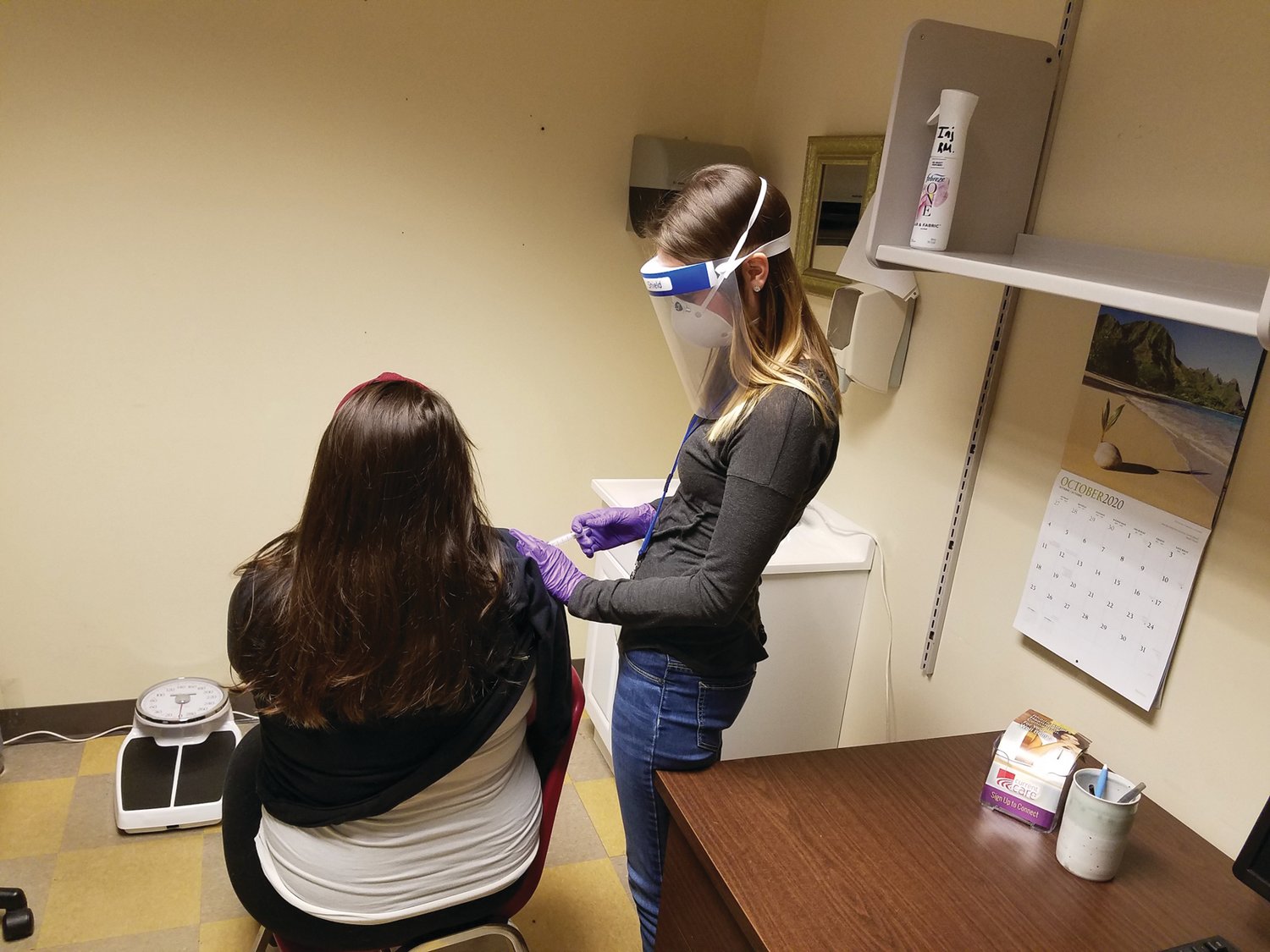
ACT Team RN Jenna O’Brien administers Haldol decanoate to a client.
With the implementation of teletherapy, staff had to adapt to providing assessments over the phone. “The biggest struggle has been losing the face-to-face connection,” stated Ana Sofia Alves, RN who works for one of Thrive’s Integrative Health Home teams. “In our field, it is important to be able to assess our clients’ affect, mood, body movements and general appearance. We rely on visual cues, which you can’t see over the phone.”

Ana Sofia Alves, RN on IHHTeam 2, discusses a client
with Sara Graham-Santilli, Community Care Nurse.
Lead Nurse Karen Rush, who has worked at Thrive for over 36 years, concurs. “For me, not being able to see clients has been the hardest,” she said. “You can tell how people are feeling and doing by watching their expressions.”
Gail Horbert, RN works in Thrive’s Housing First RI office in Providence, connecting people experiencing homelessness to permanent housing. “Our members are a very vulnerable population,” she stated. “Most of them have no one to advocate for them medically, and many have not seen a doctor in years. They don’t recognize their need for medical care, or follow through with getting it, without our support.”
Being in a high-risk category of contracting the virus, Horbert now works from her home office. “I really feel that working from home gives me the opportunity to provide undivided attention to clients without distractions,” she said. “I now have the time to earn their trust by completing nursing assessments and having the opportunity to follow through with the medical care that is so desperately needed. I am grateful to be able to work with them from start to finish. It’s so rewarding to see them in a better place.”
While Thrive’s 16- to 25-year-old Healthy Transitions clients have taken teletherapy in stride, staff are concerned many aren’t taking the threat of COVID seriously. “The young adults that I work with believe they are invincible and COVID won’t affect them personally,” said Julie Hendrickson, RN. “I keep telling them to wear masks, avoid large gatherings with friends, and stay home if they are not feeling well.”

Healthy Transitions Nurse Julie Hendrickson conducts medication reconciliation and packing for clients.
Another challenge for staff has been navigating the systems of outside providers such as labs, pharmacies, and primary care providers. “If a client complains of cold symptoms, we can’t get them to their PCP or walk-in clinic because these services aren’t allowing symptomatic folks into the office,” stated Lead Nurse Kelly Hughett. “They must get COVID tested before being seen, and transportation is an issue for our folks.”
While people on Medicaid can utilize non-emergency medical transportation services, appointments must be scheduled 24-48 hours in advance. “The things that pop up overnight like not having groceries are still a struggle, especially in West Warwick where clients don’t have a place to walk to get them,” said Jenna O’Brien, a member of Thrive’s Assertive Community Treatment Team. “Trying to get food to them has been a big challenge.”

Jenna OBrien, RN and ACT Team RN Tony Macro
reconcile medications for clients.
“Before COVID, we would take them to their cardiologist or dermatologist, wherever they needed to go,” stated O’Brien. “Now, we have to pick and choose which are the most important. When I transport someone, they are less than six feet away from me. The next person will be sitting in the exact same spot, in the same enclosed car. If one of us is exposed and takes out the whole ACT team, who will bring clients their meds and meet their needs?”
Many of Thrive’s nurses believe that case managers are COVID’s real unsung heroes. Their duties include visiting clients’ residences to assess their symptoms, ensuring their needs are met, and facilitating their coordination of care. Because their wages are tied to Medicaid reimbursement rates that haven’t increased in over a decade, many make close to minimum wage.
“I initially thought some case managers would say, ‘I can’t do this,’ but they just keep showing up for work,” shared Mary Kenney. “As a nurse, I signed up for this; they don’t get paid what I get paid. They put their lives on the lines every day. And that has amazed me.”
Thrive was able to provide case managers with hazard pay funded through COVID response grants issued by the Rhode Island Foundation, the United Way and the state of Rhode Island. These funding streams, however, quickly ran dry.
“The loss of the hazard pay has been a real blow to them,” continued Kenney. “The pay they get is not enough for the work they do, and now they have all these additional responsibilities because of COVID. A lot of our case managers have bachelor’s degrees, and they make maybe $15 an hour. They can barely afford to live.”
No matter how many obstacles Thrive’s direct line staff have overcome, they remain motivated by witnessing clients achieve major development milestones.
“In the beginning we were concerned about our ACT clients, who are isolated to begin with, would do very poorly,” said Jenna O’Brien. “Before COVID, our clients would wait until we showed up to their appointments to tell us what they needed. Now, they’re reaching out more by phone, making their needs known. We are witnessing adaptability and resiliency of the human experience that none of us have ever seen before.”
“One of my clients received Certified Nursing Assistant services from another agency in her home four days a week,” continued O’Brien. “When COVID started, her CNA needed to be home with her children. Because that agency was so slammed with cases, they couldn’t give her another one. That client learned how to cook, to clean, and to bathe herself. Her independence has flourished. Now that we know they can handle some of these situations, that when push comes to shove, they can get to the grocery store on their own, I think we will begin to gently push more for their independence, challenging them to grow.”
Others are empowered by the ways Thrive’s community members have pulled together.
“Watching our clients and staff rise to the challenge has been the most positive and heartwarming experience I’ve ever had,” said Kelly Hughett. “Yes, it takes extra time and creativity to help our folks get their needs met, but we are doing it! To see people truly care about the health and safety of others, to see them handling all the inconveniences with grace, gives me hope.”
Article Links
Sarah Channing is Director of Development & Digital Media for Thrive Behavioral Health.
